Overview
Keratoconus Is A Progressive Eye Disease In Which The Normally Round Cornea Thins And Begins To Bulge Into A Cone-Like Shape. This Cone Shape Deflects Light As It Enters The Eye On Its Way To The Light-Sensitive Retina, Causing Distorted Vision.
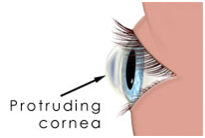
The Cornea Is The Window Of The Eye. Light Travels Through The Cornea Past The Lens To The Retina And Then The Brain To Form A Visual Image. The Normal Corneal Surface Is Smooth And Aspheric I.E. Round In The Center, Flattening Towards Its Outer Edges. Light Rays Passing Through It Moves In An Undistorted Manner To The Retina To Project A Clear Image To The Brain.
Keratoconus Typically Commences At Puberty And Progresses To The Mid Thirties At Which Time Progression Slows And Often Stops. Between Age 12 And 35 It Can Arrest Or Progress At Any Time And There Is Now Way To Predict How Fast It Will Progress Or If It Will Progress At All. In General Young Patients With Advanced Disease Are More Likely To Progress To The Point Where They May Ultimately Require Some Form Of Surgical Intervention.
The Progression Of Keratoconus Is Unpredictable But Generally The Condition Progresses Slowly And Can Cease At Any Stage. While Keratoconus Interferes With The Clarity Of A Person's Sight It Rarely Causes Blindness And In Its Early Stages, Keratoconus Causes Slight Blurring And Distortion Of Vision And Increased Sensitivity To Glare And Light. As The Disorder Progresses The Degree Of Vision Obtained Through Glasses Becomes Less Acceptable And Contact Lenses Often Become The Best Method Of Correcting Vision Problems.
Keratoconus Is A Degenerative Disease Of The Cornea That Causes It To Gradually Thin And Bulge Into A Cone-Like Shape. This Shape Prevents Light From Focusing Precisely On The Macula. As The Disease Progresses, The Cone Becomes More Pronounced, Causing Vision To Become Blurred And Distorted. Because Of The Cornea's Irregular Shape, Patients With Keratoconus Are Usually Very Nearsighted And Have A High Degree Of Astigmatism That Is Not Correctable With Glasses.
Keratoconus Is Sometimes An Inherited Problem That Usually Occurs In Both Eyes.
What Causes Keratoconus?
The Characteristics Of Keratoconus Have Been Known For At Least 200 Years, But The Specific Causes Are Still Undetermined.
Several Theories Have Been Proposed : -
- One Scientific Theory Is That Keratoconus Is Genetic In Origin. About 7% Of Patients Have Other Family Members With The Disease.
- Another View Holds That Keratoconus Is A Degenerative Condition Perhaps Linked To The Altered Balance Between Enzymes And Inhibitors Within The Cornea
- Keratoconus May Also Be Secondary To Some Disease Processes.
- A Hypothesis Has Also Been Proposed That Keratoconus May Involve The Endocrine System (Hormones) Since The Condition Is Often Diagnosed In Young People At Puberty Or In Their Late Teens.
While The Exact Cause Of Keratoconus Has Not Yet Been Determined, Research Into Keratoconus Continues And New Treatment Options Are Continually Under Development.
Signs And Symptoms
- Nearsightedness
- Astigmatism
- Blurred Vision - Even When Wearing Glasses And Contact Lenses
- Glare At Night
- Light Sensitivity
- Frequent Prescription Changes In Glasses And Contact Lenses
- Eye Rubbing
Detection And Diagnosis
Keratoconus Is Usually Diagnosed When Patients Reach Their 20's. For Some, It May Advance Over Several Decades, For Others, The Progression May Reach A Certain Point And Stop.Keratoconus Is Not Usually Visible To The Naked Eye Until The Later Stages Of The Disease. In Severe Cases, The Cone Shape Is Visible To An Observer When The Patient Looks Down While The Upper Lid Is Lifted. When Looking Down, The Lower Lid Is No Longer Shaped Like An Arc, But Bows Outward Around The Pointed Cornea. This Is Called Munson's Sign.
Special Corneal Testing Called Topography Provides The Doctor With Detail About The Cornea's Shape And Is Used To Detect And Monitor The Progression Of The Disease. A Pachymeter May Also Be Used To Measure The Thickness Of The Cornea.
Treatment Of Keratoconus
In Most People, The Cornea Will Stabilize After A Few Years Without Ever Causing Severe Vision Problems. Treatment Of The Visual Defect May Involve The Use Of Hard Contact Lenses As A Temporary Measure. The Only "Cure" Is Corneal Transplant (Penetrating Keratoplasty Or Epikeratoplasty).For Patients With No Scarring Near The Center Of The Cornea, Another Option May Be Surgically Grafting A Layer Of Epithelial Cells To Flatten The Cone-Shaped Cornea In A Process Called Epikeratophakia. It Has Results Comparable To Corneal Transplantation And, If It Is Unsuccessful, It Can Be Followed By Corneal Transplantation.
Genetic Counseling May Be Of Benefit For Patients With An Inherited Form Of Keratoconus.
In Early Stage Keratoconus, Distortion Of Vision Can Be Treated Using Glasses To Correct Minor Myopia (Nearsightedness) And Astigmatism Caused By The Condition. As Keratoconus Advances, Gas Permeable (GP) Contact Lenses Are The First Choice To Correct Vision. Most Of The Time, This Is A Permanent Remedy.
The Rose K Lens Has A Number Of Features That Make It Ideal For Keratoconus And Is Internationally Recognised As The Leading Lens For The Treatment Of Keratoconus.
- The Lenses Are Designed Using Complex Computer Models And Manufactured On Special Computerized Lathes.
- The Complex Geometry Of Rose K Lenses Take Into Account The Conical Shape Of The Cornea In All Stages Of The Condition.
- Lenses Can Be Customised To Suit Each Eye And Can Correct The Myopia And Astigmatism Associated With The Condition.
- Rose K Lenses Allow The Cornea To 'Breathe' Oxygen Directly Through The Lens Material Providing Excellant Health To The Eye.
- The Lenses Are Easy To Insert, Remove And Clean.
For more information, medical assessment and medical quote
as email attachment to
Email : - info@wecareindia.com
Contact Center Tel. (+91) 9029304141 (10 am. To 8 pm. IST)
(Only for international patients seeking treatment in India)